China's optimization of COVID-19 policies





Editor's note: China has actively optimized and refined its COVID-19 response as the pathogenicity of the Omicron virus weakens, the vaccination rate rises and the country accumulates experience in containing the virus. Following the adjustment, China's COVID-19 prevention and control efforts will focus on protecting health and preventing severe cases. Four experts share their views on the issue with China Daily.
Future of online diagnosis, care promising
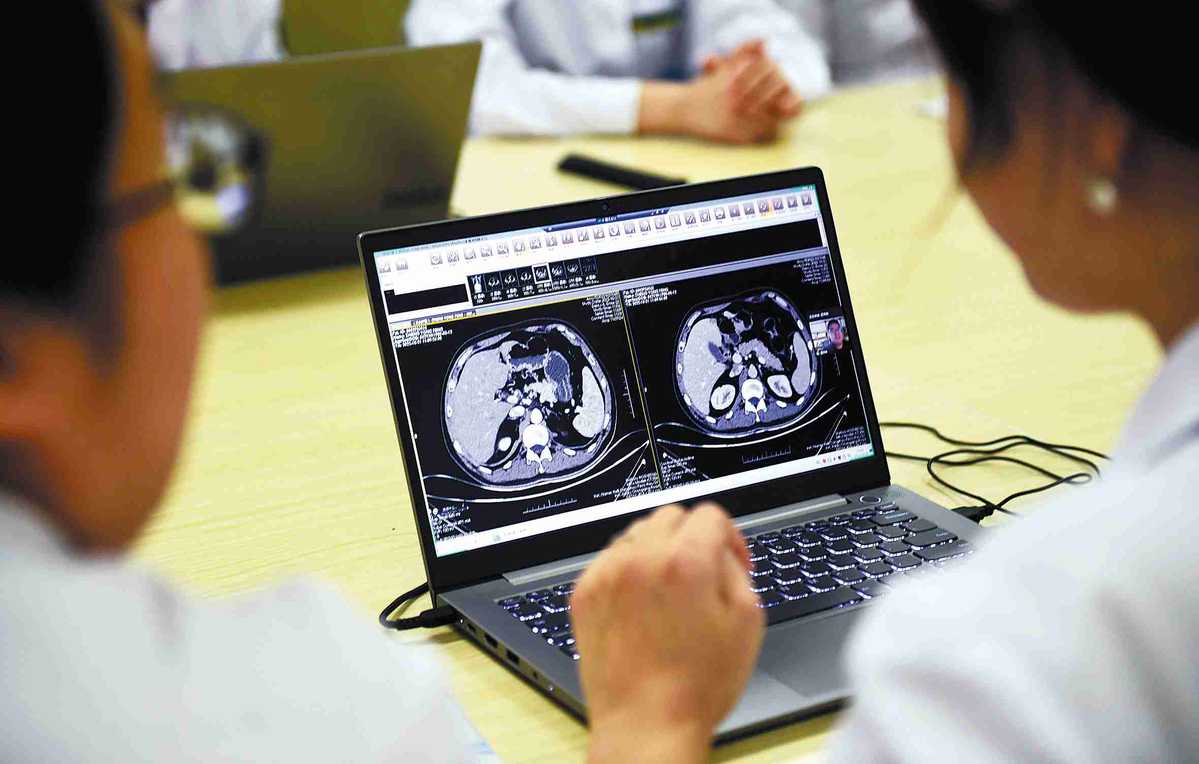
The Chinese government issued a series of supportive policies to promote the development of telemedicine much before the outbreak of the COVID-19 pandemic. The General Office of the State Council, China's Cabinet, issued the "Guiding Opinions on the Promotion and Standardization of Application and Development of Big Data for the Healthcare Industry" in June 2016 and the "Opinions of the General Office of the State Council on Promotion and Development of the Internet Plus Healthcare" in April 2018, which facilitated the establishment of the service provision system, support guarantee system, and helped make internet-aided diagnosis and treatment safer.
There was a rapid increase in the demand for internet-aided diagnosis and treatment after the COVID-19 pandemic broke out in early 2020, prompting the National Health Commission to encourage people to pay follow-up visits to online hospitals for the treatment of some common and chronic diseases, as well as to purchase medicines to curb the spread of the novel coronavirus.
At the end of 2022, the number of COVID-19 infections rocketed in China, putting huge pressure on offline medical institutions. So the NHC asked hospitals to prescribe online medical care for patients receiving treatment at home.
Internet-aided diagnosis and treatment have played a positive role in the fight against the pandemic. To start with, they have met the medical needs of many people and prevented cross-infection. During the pandemic, the online outpatient platforms provided exemplary service for the elderly, children and patients with high risk of cross-infection who could not consult a doctor in person due to the strict prevention and control measures. They also helped free offline hospitals' diagnosis and treatment resources, which were used to treat seriously ill patients.
Major hospitals have opened online COVID-19 clinics where patients can consult doctors, purchase medicines, and receive rehabilitation training. Thanks to the online medical services, many doctors who cannot be physically present at a hospital can provide online medical services.
From Dec 12 to 31, online hospitals in Guangdong province served a total of 1,246,800 person-times, attending on average 62,400 patients a day. This is equal to eight medium and large tertiary hospitals attending to 8,000 person-times a day in outpatient and emergency departments.
During the pandemic, many hospitals expanded online medical services, from online follow-up visits to non-contact medicine delivery.
However, internet-aided medical diagnosis and treatment have been caught in a bottleneck. First, the definitions of the core concepts such as common diseases and follow-up visits for chronic diseases are not clear enough, so it is not possible to standardize doctors' practice and ensure the accuracy of online diagnosis and the efficacy of internet-aided treatment.
The threshold for opening more online hospitals (public tertiary hospitals and above) is relatively high, because it requires huge investments and requires doctors (attending physicians, consultants and surgeons) to put many extra hours at their job.
Therefore, it is difficult for grassroots medical institutions to operate online hospitals on their own. While the large number of patients with mild symptoms that junior doctors can deal with is most suitable for online treatment, the State should introduce supporting policies to encourage doctors working at the grassroots level to join the service team of online hospitals.
Second, there are restrictions on patients' "first visit" to an online hospital. The NHC has set a redline for online hospitals that "do not carry out Internet diagnosis and treatment activities for first-visit outpatients", which greatly limits the value of internet-aided diagnosis and treatment. In December, however, Guangdong province took the lead in allowing the first online diagnosis of COVID-19, which was a major breakthrough.
Third, the online medical bill settlement system using medical insurance remains a problem. Take Beijing for example. Although the internet-aided diagnosis and treatment covered by medical insurance in Beijing was included in the medical insurance reimbursement system in April 2020, patients can only settle bills for medical services online. To pay the bills for treatment and medicines, they have to visit the medical institutions in person.
And fourth, the pricing of internet-aided diagnosis and treatment services is problematic, too, because they break the time and space barriers, allowing medical institutions to maximize their resource advantages. The majority of medical workers have to work beyond working hours, even outside their hospital, and a large number of senior doctors divide their time between offline and online hospitals.
Also, the diagnosis and treatment services are priced unreasonably, and don't fully reflect the work of medical workers, which is not conducive to the expansion and improvement of internet-aided medical services. So appropriate measures should be taken to unleash the full potential of online hospitals.